
CLICK THE LINK
Limbal relaxing incisions (LRI’s)- Correct Astigmatism
LRI’s are a minimally invasive surgical procedure used to treat low to moderate degrees of astigmatism, often performed in conjunction with cataract surgery to help patients achieve clear vision with a reduced or eliminated need for glasses or contact lenses.
LRI’s are tiny cuts made around the edge of the cornea, called the limbus, which “relax” the cornea’s steep curvature and improve the way the eye focuses light. Compared to other procedures performed to correct astigmatism, such as astigmatic keratotomy, LRI’s heal faster and cause fewer side effects. The incisions can either be made manually with a diamond blade or with a Femtosecond Laser at the time of laser cataract surgery.
This procedure is ideal for patients with astigmatism seeking to improve their vision at all distances. It is important for patients to be in good overall health and to have realistic expectations for surgery before undergoing this procedure. While most patients experience significant improvements to their vision after LRI, some may still require vision assistance in the form of glasses or contacts.
Watch Dr. Kavanagh perform an LRI at the slit lamp to fix astigmatism.
Corneal Transplantation
The cornea is the clear covering of the front of the eye which bends, or refracts, light rays as they enter the eye. For clear vision to occur, the cornea must have the correct shape and clarity to focus incoming light rays precisely on the retina at the back of the eye. When the cornea becomes cloudy or misshapen from injury, infection or disease, transplantation may be recommended to replace it.
Descemet’s Stripping Endothelial Keratoplasty
Descemet membrane endothelial keratoplasty (DSEK), is a surgical procedure that removes the abnormal inner lining of the cornea, known as the endothelium, replacing it with a donor cornea.
Endothelial keratoplasty is performed through a much smaller incision than regular cornea transplantation resulting in shorter recovery time and with fewer risks than a traditional corneal transplant. Recovery of vision is quicker with endothelial keratoplasty and there is less of a restriction on activities. There is less of an issue with astigmatism in an endothelial keratoplasty and there are minimal or no suture problems.
Penetrating Keratoplasty (PKP)
Penetrating keratoplasty (PKP) replaces the entire thickness of the cornea with a donor graft. The new cornea is stitched into place, and stitches are usually removed after a year. It may take this long for vision to be restored to satisfactory levels as well, requiring many patients to wear glasses or contact lenses after this full thickness corneal transplant procedure.
With the development of technological advances, PKP is not performed as often as the other types of corneal transplant procedures. Your doctor will determine whether or not this procedure is right for you after a thorough evaluation of your eyes and any pre-existing conditions.
What are the causes of Corneal Damage:
It is important to have a healthy cornea for clear vision. The cornea is located on your eye’s outer surface and is responsible not only for protecting your eye from foreign debris but also for helping focus light that enters your eye. Because the cornea is so “front and center” on the eye, it is also prone to get damaged, diseased or scarred due to:
- Trauma
- Allergies
- Inflammation (keratitis)
- Infection
- Dry eye
- Cone-shaped cornea (keratoconus)
- Loss of Endothelial Cells (Fuchs ‘ dystrophy)
- Protein deposits (corneal dystrophy)
- Shingles
- Ocular herpes
- Pterygium
If glasses or contact lenses for daily tasks cannot restore your vision, a corneal transplant may be recommended by your doctor. This process works by removing all or part of the cornea and substituting it from an eye bank with healthy donor tissue. This is the most common tissue transplant, and eye banks usually have donor corneas on demand, so there is not usually a “waiting list” for this type of surgery.
Our corneal experts, Dr. Kavanagh, and Dr. Psolka can perform corneal transplants at Eye Associates of South Texas. We may recommend a: full-thickness corneal transplant (penetrating keratoplasty or PK) to replace the whole cornea, depending on the severity of your problem. To keep the new cornea in place as the eye heals, temporary sutures are needed. Partial thickness corneal transplant (Descemet’s Automated Stripping Endothelial Keratoplasty or DSAEK) that replaces the damaged section of the cornea’s inner back layer. Few sutures are required and faster visual recovery is achieved by most patients.
If you are considering corneal transplantation, make sure that you are fully aware of the risks of surgery such as rejection of new tissue, infection, and corneal swelling. Trusting your eyes to experienced ophthalmologists like the Eye Associates of South Texas surgeons will help to reduce some of these risks. To schedule an appointment with one of our highly skilled doctors, contact Eye Associates of South Texas at 830-379-3937.
Pterygium
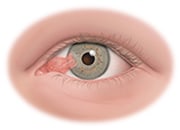 Pterygium is a painless, non-cancerous growth of the conjunctiva, the lining that covers the white part of the eye. The pterygium may grow on the cornea, which covers the iris, the colored part of the eye. It can be red, pink, white, yellow, or gray in different colors. Patients with pterygium often first notice the condition due to the appearance of an eye lesion or dry, itchy irritation, tearing or redness. Usually, the pterygium is first noticed when confined to the conjunctiva only. It’s called a pingueculum at this stage. It is called a pterygium once it extends to the cornea and can eventually lead to vision impairment. In mild cases of pterygium, artificial tears can be used to reduce the dryness and irritation it causes.
Pterygium is a painless, non-cancerous growth of the conjunctiva, the lining that covers the white part of the eye. The pterygium may grow on the cornea, which covers the iris, the colored part of the eye. It can be red, pink, white, yellow, or gray in different colors. Patients with pterygium often first notice the condition due to the appearance of an eye lesion or dry, itchy irritation, tearing or redness. Usually, the pterygium is first noticed when confined to the conjunctiva only. It’s called a pingueculum at this stage. It is called a pterygium once it extends to the cornea and can eventually lead to vision impairment. In mild cases of pterygium, artificial tears can be used to reduce the dryness and irritation it causes.
Although the causes of pterygium are not fully known, exposure to UV light is believed to be the main cause. Living in a dry, dusty, windy environment is another suspected risk. Therefore, people living near the equator or playing water sports like surfing and fishing are more likely to develop pterygium. They are especially common in South Texas, where the doctors of Eye Associates of South Texas have extensive experience in the surgical removal of the growths. Long-term exposure to these conditions causes thickening of the conjunctive and redness and irritation of the eye. Collagen starts to deteriorate in the eye and the eye is weakening. Studies show that genetic predisposition to pterygium may also occur, with a higher prevalence in men compared to women. Pterygium symptoms and signs include dryness, redness, irritation, inflammation, and tearing. The pterygium may grow over the pupil in more severe cases and limit vision.
Sunglasses that block UV rays are a good way to protect against pterygium, especially sunglasses that provide side coverage. Wiley X sunglasses are ideal they are available from Eye Associates of South Texas opticals, as they block UV light coming in from the side of sunglasses due to their unique wrap-around design. It’s also helpful to wear a hat with a brim to block sunlight. Artificial tears (eye drops) should be used in hot, dry climates to help lubricate the eyes.
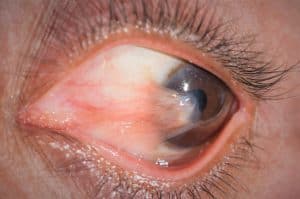
Pterygium
Pterygium Removal (Surgery)
For patients with severe cases of pterygium and whose vision has been affected, a surgery known as a pterygiectomy is the only way to definitely remove this growth. This may be achieved through two different types of surgical procedures, either using tissue taken from another part of your body or an amniotic membrane graft.
Watch Dr. Kavanagh perform a pterygium excision with conjunctival autograft and application of MMC. Also includes Day One postoperative appearance.

