
CLICK THE LINK
Dry Eye
 Dry eye is a common condition that occurs when the eyes are insufficiently moisturized, leading to itching, redness and pain from dry spots on the surface of the eye. The eyes may become dry and irritated because the tear ducts don’t produce enough tears, or because of a chemical imbalance in the tears.
Dry eye is a common condition that occurs when the eyes are insufficiently moisturized, leading to itching, redness and pain from dry spots on the surface of the eye. The eyes may become dry and irritated because the tear ducts don’t produce enough tears, or because of a chemical imbalance in the tears.
Patients with this condition often experience irritating symptoms and which may result in more serious damage to the vision if the condition is left untreated. It is important for patients with this condition to take special care of their eyes in order to alleviate symptoms and prevent complications. Your doctor can diagnose dry eye after a thorough evaluation of your eyes and tear production with the TearLab’s osmolarity testing unit.
TearLab Osmolarity system for the diagnosis and management of Dry Eye patients is the first objective and quantitative test. The literature describes hyperosmolarity or increased sodium in the tears as a primary marker of the integrity of the tear film. Your doctor will take a small sample of tears and measure tear osmolarity from both eyes. Your Osmolarity Number provides a significant health and stability measurement of the protective tear film covering the eye surface. The figure corresponds to the seriousness of the disease. You will measure your osmotic number in order to track your progress once again if you have been placed on the Dry Eye Disease Treatment Plan.
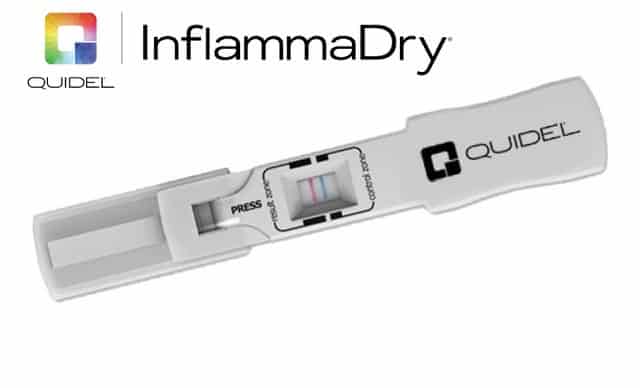
INFLAMMADRY ® This is one of our dry eye exam tests at Eye Associates of South Texas. The symptoms often lag behind clinical signs of dry-eye disease. Inflammation, especially a molecule called metallomatrixproteinase-9 (MMP-9), is one of the markers for dry-eye disease. InflammaDry detects an increased level of MMP-9 during other dry eye trials to determine whether the symptoms of your drought are caused by active inflammation around the eyes and the dry eye symptoms. High MMP-9 also can be related to systemic disorders such as Sjogren’s or other rheumatological disorders. We can recommend anti-inflammatory therapy, including steroid drops, Restasis ®, or Xiidra ®, depending on the results of the InflammaDry trial. InflammaDry’s results can also help us monitor your treatment response over time.
Causes of Dry Eye
People usually begin experiencing dry eye symptoms as they age, but the condition can also result from certain medications, conditions or injuries. Dry eye tends to affect women more often than men, due to the hormonal changes that take place during pregnancy or menopause. Oral contraceptives can also affect the consistency of tears. Dry eye is more common in people over the age of 50. Other causes of dry eye may include:
- Aging
- Medication such as antihistamines, decongestants, blood pressure medication and antidepressants
- Medical conditions such as rheumatoid arthritis, diabetes and thyroid problems
- Environmental conditions such as smoke, wind, air conditioning, and dry climates
- Long-term contact lens use
- Eye surgery
- Sun exposure
- Smoking or second-hand exposure to smoke exposure
- Sjogren’s syndrome
- Thyroid eye disease
- An eye injury
- Eyelid surgery
- Inflammation of the conjunctiva
- Exposure keratitis
These factors can affect the frequency or consistency of tears, both of which can lead to dry eyes. Our natural tears require a certain chemical balance in order to efficiently moisturize the eyes.
Dry eye occurs when the eyes fail to produce the correct amount of tears or quality. Tear production can decline with age, females especially post-menopausal are affected more than males, likely due to hormonal changes.
Dry Eye is one of the least understood conditions of the eye that affects so many people. Many people with dry eyes blame the weather, eye-strain, allergies for their symptoms. Although all these can worsen the symptoms of Dry Eye, it is not the cause. In order to maintain and protect the eye’s surface, your eyes need a constant layer of tears, which is called a “tear film.” The tear film is composed of three layers: Mucin, Aqueous and Lipid. In Dry Eye, changes in the health of the tearing or lacrimal glands can lead to a change in the quantity and quality of your tears. Furthermore, the Meibomian Glands, which produces lipids (oils) on the margins of your upper and lower eyelids, prevent your tears from evaporating. All these glandular changes and inflammation lead to a tear film which can no longer give your eye sufficient nutrition or protection. This leads to burning or foreign body sensation, excessive tearing, blurred vision, redness and eventually chronic dry eye disease. If left untreated, your eyes will change continuously and become hard to improve with conservative treatment. Drs. Kavanagh, Acosta, Ehiem, Jacob, Hammodeh, and Psolka are specialists in Dry Eye Diseases in San Antonio, New Braunfels, Seguin, and La Vernia TX. They have treatments for the mildest to most severe dry eye both aqueous deficient and evaporative types.
The Eye Associates of South Texas also offers comprehensive tests, including Inflammadry ® tests that can detect a significant inflammatory marker (MMP-9).
Dr. Acosta has spearheaded the Dry Eye Clinic at the Eye Associates of South Texas, we have meibomian gland imaging at both San Antonio, Seguin, and New Braunfels locations. LipiFlow is available at all our locations.
Symptoms of Dry Eye
Patients with dry eye may experience certain symptoms from this condition, usually affecting both eyes, which may include:
- Stinging or burning sensation
- Irritation from smoke or wind
- Eyes that feel scratchy
- Eye fatigue
- Sensitivity to light
- Difficulty wearing contact lenses
- Excessive tearing
- Blurry vision
Dry eye can damage the eye’s tissues leaving tiny abrasions on the surface of your eyes, impairing vision. Fortunately, many treatment options are available to help relieve the symptoms of dry eyes, restoring health back to the eyes ensuring clear vision and long-term health.
Complications of Dry Eye
Left untreated, dry eye can lead to the following complications:
- Pain
- Ulcers or scars on the cornea
- Loss of vision
Treatment of Dry Eye
Treatment for dry eye depends on the cause and severity of the condition, as well as the patient’s overall health and personal preference. Non-surgical treatments are often effective, and may include the following:
- Blinking on purpose
- Increasing humidity levels at home or work
- Use artificial tears or a moisturizing ointment
- Stop smoking or exposure to second-hand smoke
- Avoiding air conditioning or windy conditions outdoors
- Stop the use of allergy and cold medicines
- Adding omega-3 fatty acids to the diet as food or supplements
- Use of Autologous Tears
If non-surgical methods are unsuccessful, surgical treatments may be an option. Treatment options may include:
- Small punctal plugs may be inserted in the corners of the eyes to limit tear drainage
- Punctal cautery, a procedure to permanently close the drainage holes may be another option
- Eyelid surgery is also a solution if an eyelid condition is causing your dry eyes
Treating the underlying cause of dry eyes can also help relieve the symptoms of this condition.
Autologous Tears
Autologous tears are a common treatment for severely dry eyes. They are prepared similar to artificial tears but are made from the patient’s own blood. Unlike artificial tears that only lubricate the ocular surface, serum tears have vitamin A, fibronectin, immunoglobulins and growth factors that promote epithelial health. Autologous tears are prepared by a tissue bank after the patient gives a sample of their blood, usually in 3 months supplies. One drawback of this therapy is that frequent blood draws are required and it’s not usually covered by your medical insurance.
Restatsis® and Xiidra
 RESTASIS® Ophthalmic Emulsion is the only prescription eye drop available for patients, who have chronic dry eye, that helps increase the eye’s ability to produce more tears.
RESTASIS® Ophthalmic Emulsion is the only prescription eye drop available for patients, who have chronic dry eye, that helps increase the eye’s ability to produce more tears.
Used according to prescription, patients who use RESTASIS® report a noticeable increase in tear production, as opposed to those using steroid drops or tear duct (punctal) plugs.
Immunosuppressives like Restasis or Xiidra increase tear production by reducing inflammation, they take weeks to months to work, and are quite expensive. But can dramatically decrease dry eye symptoms, and give patients significant relief. These treatments actually increase the amount to tear production, versus saving the natural tear formation.
Restoration of the Ocular Surface to Improve Severe Dry Eyes- Amniotic Membrane

Aril is a dehydrated amniotic membrane placed under a bandage contact lens. It can be used for many different conditions, including abrasions of the cornea, herpetic ulcers, recurrent corneal erosions, keratitis, chronic dry eyes. In severely dry eyes, with corneal damage and failure of conservative treatment. Your eye doctor may place a dehydrated amniotic membrane in one eye at a time and it can stay in your eye for one to two weeks, under a bandage contact lens. The length of time depends on the dry eye’s severity. It helps your eyes through the healing properties of the amniotic membranes. In addition to regenerative properties, the amniotic membrane has anti-inflammatory properties to grow new healthy cells. This will increase the ability of the eye to heal more quickly and reduce pain as well. In essence, the corneal cells affected by chronic dry eye can heal and regenerate for better, healthier cells. While the amniotic membrane is in your eye, you can still use eye drops. Your ophthalmologist at Eye Associates of South Texas will have you back to remove the contact lens once the amniotic cells have an opportunity to contour your eye. Amniotic cells differ from stem cells as amniotic cells are taken naturally after pregnancy and no harm is done to anybody to get these cells.
Watch Dr. Kavanagh treat a painful corneal erosion with Amniotic Membrane.
Please call Eye Associates of South Texas at 830-379-3937 to schedule an appointment if you have any of the symptoms of dry eyes.
Treatment of Meibomian Gland Disease (Major Cause of Evaporative Dry Eyes)
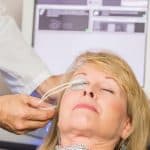
Lipiflow® BY Johnson and Johnson
You may be a candidate for this exciting technology if your dry eye disease is determined to have a glandular component of the eyelid. LipiFlow ® is a new method designed to deal with the root cause of the blocked Meibomian gland Evaporative Dry Eye. Once open and clear these blocked glands can enable natural lipid (oil) production needed for a healthy tear film to resume. Some treatments try to add more liquid to the tears, but tears continue to evaporate more quickly than they are produced without the complex natural oil. Your doctor will look at your eyelids and eye surface in a clinic and see if the tear film health is poor. If you are determined to be a good candidate the lipiflow treatment will be carried out. The treatment is simple, in a quiet room the activator is placed between the cornea and external eyelid. This design allows thermal heating to be placed opposite the exterior of the eyelid to the back surface of the Meibomian glands. The Thermal Pulsation System compresses the glands, and this clears the contents as the glands are softened. This can restart your body’s natural lipid production (oils) required for your healthy tear film. The single-use design and integrated sensors of the Activator guarantee safe, sterile treatment. This can make you forget about burning, red, tired dry eyes.
BlephEx
BlephEx is an in-office painless procedure to treat blepharitis. It utilizes a patented handpiece with disposable tips that clean and exfoliate the eyelid margin and remove scurf with a rotating medical grade micro-sponge. This treatment is carried out in about 6-8 minutes by one the Eye Associates of South Texas Eye Doctors or by one of their certified technicians. The eyelid margin must be clean of debris and scurf so that the meibomian glands may produce their meibum that added to the tear film stops the evaporative type of dry eye disease. BlephEx of the eyelids by your eye doctor is analogous to teeth cleaning by your dentist and should be repeated every 6 months. In between BlephEx treatments nighttime lid hygiene should be carried out, this is akin to flossing your teeth. This will keep your eyelid margins healthy and may decrease the chances of getting: dry eyes, blepharitis, chalazions or styes.
IPL by Lumenis M22 with OPT (Optimal Pulse Technology)
Intense pulsed light therapy (IPL) in patients for whom no other therapy has worked is often successful. A physician at Eye Associates of South Texas can help you decide if IPL will help your dry eye disease. IPL stands for Pulsed Light Intense. IPL therapy relieves many and dramatically improves the comfort of your eyes. This treatment has been shown to reduce or eliminate dry-eye symptoms and has helped many people return to a normal, dry-eye-free life. For years, IPL therapy was used for purposes other than dry eye relief. Dermatologists have used this FDA-approved method to reduce redness and improve skin appearance for acne and rosacea patients, as well as to decrease skin bacteria. Research has shown that IPL also works to treat dry eyes patients and reduce their symptoms of dry eye. The treatment itself is simple, one of our board-certified ophthalmologists will direct intense pulsed light bursts at your lower eyelids, cheeks, the whole width of your face with IPL therapy. In these areas, the blood vessels absorb light and heat, causing an opening of the tear glands. Doctors can express the glands of clogged secretions once the glands are open, allowing them to work properly again. This rapid 15-minute procedure is performed in the clinic. The number of recommended treatments depends on the patient. Typically, most patients receive five treatments in the first six months. Right after the first treatment, it is common for patients to feel relief. Maintenance treatment is recommended every 6-12 months.
Preventing Dry Eye
There are certain steps patients can take to prevent the symptoms of dry eye from occurring, which is especially useful for those at an increased risk of developing symptoms. Simple lifestyle modifications such as wearing protective glasses on windy days, giving your eyes a break during reading or other strenuous tasks can effectively reduce the frequency and severity of symptoms.
Your doctor will provide you with instructions as to how you can avoid the symptoms of dry eye based on your individual condition.
Blepharitis
Blepharitis is the chronic inflammation, or infection, of the eyelids and the eyelash follicles along the edge of the eyelid. Blepharitis, which is not contagious, affects patients of all ages.
Causes of Blepharitis
There are several reasons for the occurrence of blepharitis, some of them are:
- Seborrheic dermatitis
- Acne
- Bacterial infection
- Allergic reaction
- Poor eyelid hygiene
- Rosacea
Symptoms of Blepharitis
Symptoms of blepharitis include:
- Red or swollen eyes
- Red or swollen eyelids
- Frequent tearing of the eyes
- Eyelids that are crusty, flaky or scaly
- Sensitivity to light
- Blurry vision
- Burning sensation in the eyes
In more serious cases, sores can form when the crusting skin is removed, the eyelashes may fall out, the eyelids can deform, the infection can spread to the cornea, and patients often suffer from excessive tearing. Blepharitis can also cause styes, chalazions, and problems with the tear film.
Diagnosis of Blepharitis
The doctor will be able to diagnose blepharitis after a thorough examination of your eyes. Some of the items examined include:
- Examining the eye
- Evaluating the margins of the eye, the eyelashes, and the oil glands
- Reviewing the medical history of the patient
Treatment of Blepharitis
There is no cure for blepharitis. Blepharitis can be controlled with proper hygiene of the eyelids. Treatment and preventative care for blepharitis involves a thorough but gentle cleaning of the eyelids, face and scalp. Warm compresses can be applied to loosen crust and gentle baby shampoo can help keep the eyelids clean. This treatment may be combined with antibiotics if a bacterial infection is causing or contributing to the condition.

